Fragility
This post hasn’t been written for you the reader, but for me the author. I’m writing this to remember, as I have been told that “in 3 to 6 months it will all feel like a dream…”.
**WARNING: Some readers may find some of the content/photos disturbing.**
Here’s the TL;DR:
This August (2014) and September I lost 19 days of my life, and for two of those 19, I almost lost my life entirely. I got the flu that progressed (quickly) into a chest infection, went to hospital, deteriorated quickly, admitted into ICU and was put on a life support machine called an ECMO. For two days it was a coin-flip whether I would survive the day. I did recover, also very quickly, but not without a significant amount of fall-out from the whole event. This post tries to detail all of this.
A lot of this post will be quotes from my fiancé’s diary that she kept.
This life-changing event started on around the 13th of August 2014 with the common flu. The flu went through its normal symptoms with sweats and shivers and aches. I thought the flu was mostly over on Friday the 15th – so much so that I felt ok drove to the other side of Melbourne to collect a rug that we had purchased. However that night things started getting worse.
I had been proactive and saw the doctor, who said “you have the Flu, get some rest”. Sage advice indeed.
I knew something was wrong when from the Thursday through to the following Tuesday I was unable to sleep… at all. Clearly this significantly weakened me to the point that I was very ill. I managed to see the doctor again on Tuesday (the 19th of August) morning and as soon as he opened his door he gave me a shocked look, said nothing other than “you’re off to hospital!”. He quickly wrote a referral and sent us on our way. We drove to Knox Private hospital nearby and, after struggling to both find and walk to the entrance, registered for my admittance. I sat down on some seats in the reception area after struggling to fill out some paperwork and was soon after collected in a wheel chair.
I vaguely remember being wheeled past reception and into a room. From there I remember nothing else until I woke up 19 days later – on the 5th of September.
My fiancé kept a diary of the days that followed, and since I have no recollection, I’m copy/pasting (edited) the events from her diary:
Tuesday, 19th August 2014 – Day 1
In the clinic the nurse gave me a brief summary, early diagnosis of pneumonia with tomorrow confirming the results. His body has extreme hypoxia, hasn’t slept four days, did not eat, extreme weakness.
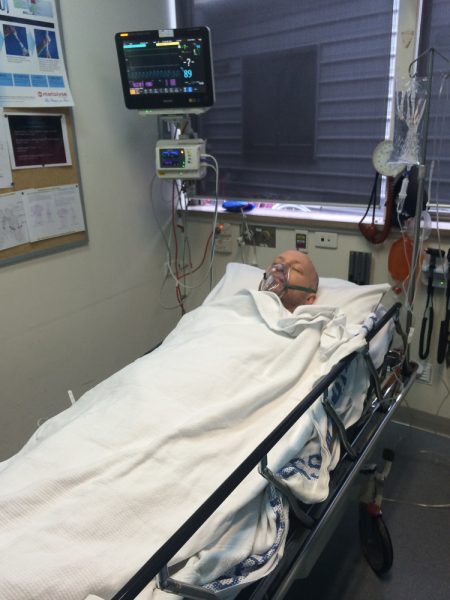
Wednesday, 20th August 2014 – Day 2
After the visit I notice he is extremely weak, the words are difficult, his temperature has reached 42 degrees. He said that he had only two hours of sleep last night sleep, it’s amazing. I waited and talked to the doctors – the most critical thing is that it’s not known what caused the pneumonia, but they will act is if it was a viral treatment needing 6-8 weeks to recover.
Thursday, 21st August 2014 – Day 3
Just went to see the doctor who told me that they were waiting for me to come, they have decided to put him on a breathing machine because his body is unable to generate oxygen content. In this process anaesthesia is applied, as well as sedation, so he can sleep for a few days. That’s good, he can finally sleep.
Friday, 22nd August 2014 – Day 4
Looking back to Tuesday, a nurse told me he had revived and sometimes will sleep. Oxygen uptake from 95% down to 75%, but progress was slow. Still a little fever, 38 degrees. Starting today, he will begin to increase his resistance to the medication, and the medication has just been increased. After entering the room, he was covered in sweat, hot on the back. He tried to communicate with the phone, but struggled to type, originally he wanted to pen and paper, the nurse tried to help by raising his bed head. He gets anxious when he wants to pull the tube out of his mouth and the nurses have to stop him.
Then the next day on Wednesday morning, I came in and the nurse told me you were not very well. You told me you had about 2 hours of sleep and it was “amazing”. You were quite emotional and told me you had crazy thoughts. You are not well at all, got high temperate of 42 degrees! It was also painful as we haven’t received the specimen result as to what is causing your bad pneumonia. Then I waited outside waiting to see the doctor. He’s the infection specialist and told me that it’ll take 6-8 weeks for you to recover in hospital, then around 2 months to recover at home.
Saturday, 23rd August 2014 – Day 5
I called ICU and they told me your condition is stable and you had a fair bit of sleep. When I arrived at the hospital I had a talk to the doctor, he said your condition is stabilised, but your recovery is very slow and will expect you in the tube and ICU for another week. So at least it’s a good news that you are getting better. When I get in and hold your hands, you opened your eyes – I know you know I was there. Your head is covered in sweat, very wet. And when I touched your back, it’s very wet too.
Sunday, 24th August 2014 – Day 6
Your nurse told me that your condition is worse than yesterday, your oxygen level went up from 50% to 80%, and your temperature went up to 38.3, then 38.9. They are doing another round of tests just to rule out that there is no new infection in your body. But she suspected that you have been resisting when changing sheets, it took your energy to recover. She gave you some Panadol as well as more sedation, so you sleep better (to save energy). I went inside and you were in a deep sleep. Your head is full of sweat. The nurse explains to me that the recovery will be fluctuating, and it’s expected that even when you are out of ICU, the recovery will be up and down as your body had undergone so much. There are so many drugs, they even induce amnesia to help you to forgot all of this trauma (no wonder you don’t know how many days you have slept). You have been sleeping for two days since Friday night – the last time I talked to you is Friday 12pm.
I called ICU to check how your condition is – the nurse told me your temperature was down to normal, and oxygen level is 70%, so it’s okay.
Monday, 25th August 2015 – Day 7
They told me a Doctor from the Alfred hospital is here today, it’ll be good if I can have a talk to him. They also told me the x-ray shows that your lung hasn’t gotten any better, actually it’s become inflamed. This virus hits young people especially hard. Your oxygen level is going up to 90% and your temperature is back to 38 degrees.
The nurse broke the news to me that you’ll be transferred to Alfred hospital this afternoon, which felt like another blow to me. I finally got a chance to talk to Doctor. He is the director in Alfred hospital ICU and he explained to me the reason for the transfer – Your oxygen level requirement is 100% now, in case during night time at 3am, you need more oxygen, and there is no way they can feed you more here in Knox. So they need to cut a hole in your leg to put a man-made lung to pump extra oxygen in your body (as your lung is too inflamed), which can only be done in Alfred hospital. He is the specialist in treating pneumonia, he had seen 80 cases during the 2008 swan flu epidemic season. He told me there are 2-3 young people in same situation as yours in Alfred. (They heard about you since you were in Knox, but at that stage your condition is not too bad to be move to Alfred). He said you’ll be in tubes for 2 weeks, or 2 days if it’s a fast recovery. His explanation made me feel better as you’ll be in the best hands. So the transfer will be 7pm tonight. They need to organise a team to come and then transport you to the Alfred hospital.
Around 4:30pm, your nurse for today called me and told me that you were transferred to the Alfred Hospital. 5 doctors came from The Alfred to help plus doctors from Knox, so it’s a big move! I regret I wasn’t there. Then around 6pm a Doctor from Alfred Hospital called me and gave an update – He explained you are doing well, settling down, and they will call me if there’s any problems.
I gave a call to Alfred ICU again to check how you are doing. They said they won’t do anything for you tonight, just let the machine work for you. You seem okay, with no sweat, are comfortable, no resisting – which is good to hear. The nurse explained to me that as the ECMO machine is working for you, your body doesn’t have to work too hard. Oxygen level is not a benchmark any more as it’s a different system now. They will check tomorrow morning to see how you are doing.
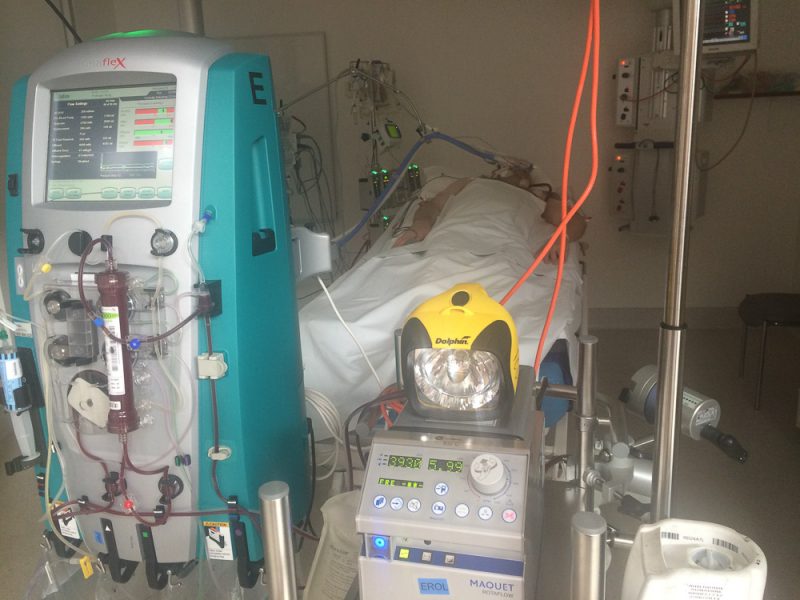
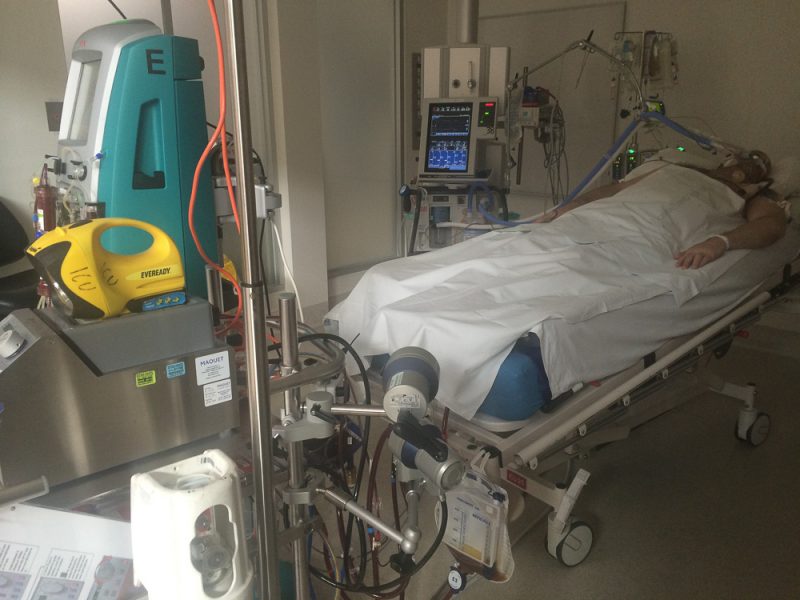
Tuesday, 26th of August 2015 – Day 8
I called the Alfred Hospital to see if there is any update. They are going to do a ultra-sound on your heart just to make sure it’s okay. The doctor will come to see you this morning to have a detailed look of you. At the moment they still define your condition as “very very sick”. The treatment for virus is over, so no need to cover our mouths when visiting you.
At 8:40pm I called ICU again to see how you doing. They said you are stable, same as you were yesterday. No change. The ultra-sound result is okay. They will be watching you in the next 24-48 hours to see which direction things will change. If it’s better, they can take off the tube in your lung, so you can wake up.
Wednesday, 27th of August 2015 – Day 9
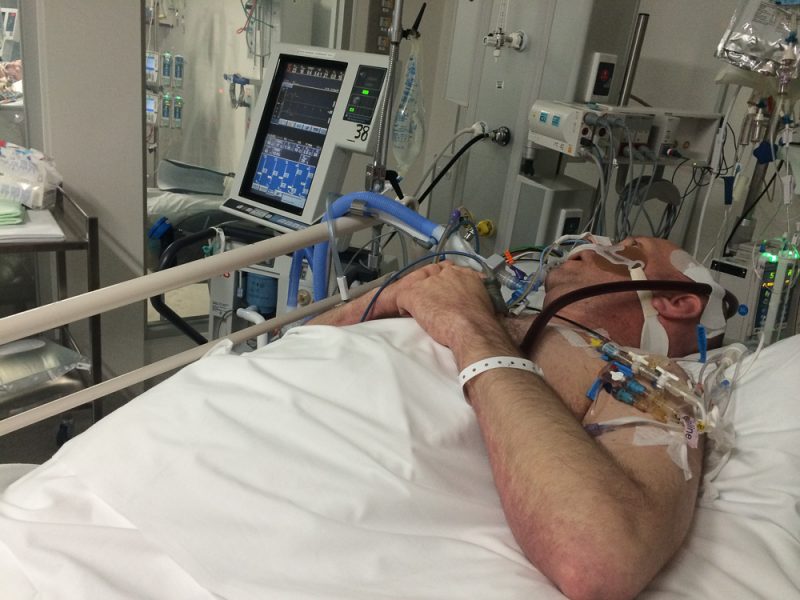
The nurse explained to me that they put another line in your neck, just to get extra line of blood to the lung machine as you need more oxygen to keep other organs working well. Your lung still is quite sick, the tube into your lung wasn’t working much comparing to the one from the lung machine.
Your skin looks a little pale, and you are lying very still. The nurse told me sometimes you coughed and try to roll over, every time you do the oxygen level goes up. That means it takes a lot of effort for your body to do it.
Thursday, 28th of August 2015 – Day 10
From both the x-ray and the machine, it showed you are improving! So they woke you up a little bit (just so you can move your hand/arm to use muscles and can hear that I came, but not too much as coughing each time consumed too much of your energy). I went to your side, and I can tell you knew I was there. You raised your hand and your eyes opened (very hard). The nurse told me to settle you, to let you close eyes and continue to sleep.
Friday, 29th of August 2015 – Day 11
It’s Friday today, has been one week since we communicated last time using paper and pen. You had a long long sleep. They said you won’t remember this experience, as medicine was given for you to forget this stressful period.
I asked how often they changed your lying position, they said it’s every 3 hours. I guess your body must feel sore. And you already got a rash on your skin – something they said related to allergy to the medicine.
Saturday, 30th of August 2015 – Day 12
Your nurse said you are moving a lot. You raised both of your hands, and tried to move your legs. You can hear us, and when I asked if you can hear us, you were nodding!
The nurse asked if you feel pain, you shook your head. When she asked if you are uncomfortable, you nodded. You don’t like the tube, and you want to move your leg, unfortunately they have to stay the way it is. So the nurse gave you more sedation and you dozed off.
One of the Doctors told me that you have improved, he’s very happy with the progress. He said currently you are breathing 50% of oxygen. The x-ray comparison also showed lots of improvement – (a few days ago it’s all white, now its half and half). They could take off the ECMO machine now, but it will hurt your lungs. So they plan to leave it for two days. (the longer to leave there, the more risk you’ll get infection, and it’s not comfortable and requires you to stay still). The doctor stressed many times that without ECMO machine you’ll die, which is true. You’ll have the tubes for longer, but depends on how you improve.
Sunday, 31st of August 2015 – Day 13
The nurse told me you had a good day. They switched off the ECMO machine, and you were really coping well. The plan is to take the ECMO machine off you tomorrow, then wake you up a little bit until your lung is totally recovered. While I was very happy with this news, they told me at the same time that your kidney and liver got infected (still by virus I think) and your white blood cells keep going up. They were treating you with antibiotics quite aggressively to try and keep the infection under control.
Monday, 1st of September 2015 – Day 14
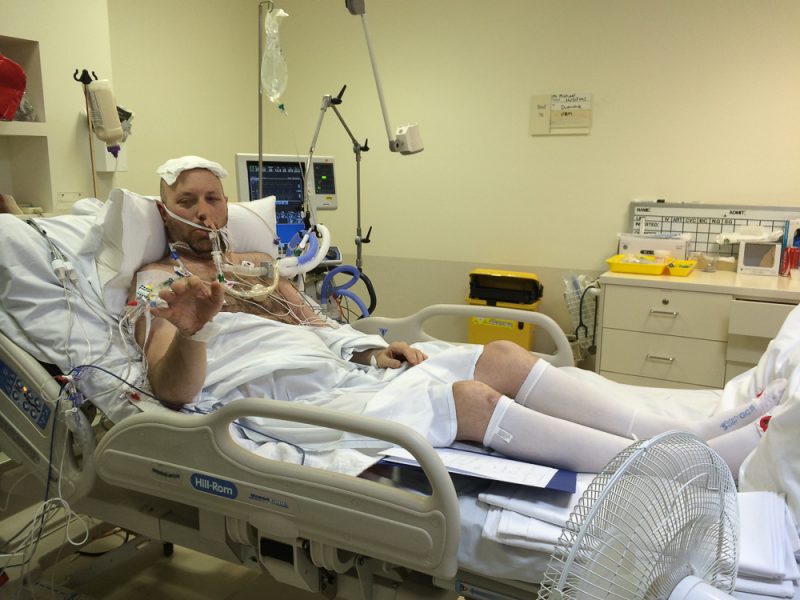
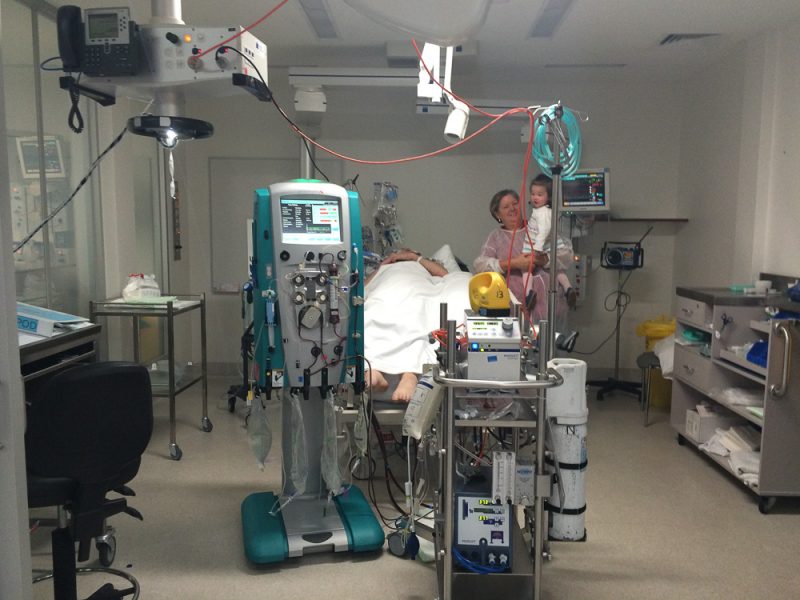
When we got in you look better, you are responding more. First you gestured for me to take photo of you, so I took photo as well as video, about you, about the machine.
I told you today is 1st of September, you are in Alfred hospital and you have been sleeping for 10 days. You looked as if taking everything in when I spoke. Sometimes you frowned hard. Then I was sent out by the nurse again as it irritated you too much.
Tuesday, 2nd of September 2015 – Day 15
The breakthrough news came at 4:30pm, when I called ICU and asked how have you been. Your nurse answered the phone and told me that they took the tube off from you today as you are recovering so well. You can talk now, and you had already sat in a chair for 10 mins today. You were a little confused this morning, but you got better this afternoon. She said the doctor was really happy with your recovery, that’s why they decided to take it off today.
Wednesday, 3rd of September 2015 – Day 16
The nurse said you were quite awake today. You are still weak as you sit by the edge of bed and felt dizzy. You had your first meal tonight with her help (which is great!). You are still quite confused as the doctor asked where you were, and you couldn’t answer. The plan is to keep you in ICU for a few more days before they transfer you to the ward, as you can have better rest there.
When I arrived at the hospital, the nurse told me that you had your teeth brushed this morning with her help. When I got in you look so small, even so tiny, but you are not connected to tubes and lines! You were half-seated and you were looking at me, only your face showed no expression. You can recognise me! And when I get close, you held my cold hand and asked me to put my hand on your eyes and you sighed with some relief “it’s so nice”.
Thursday, 4th of September 2015 – Day 17
I called ICU around 5pm to see how you doing. The nurse told me that you had about one hour sleep. I talked to the doctor, he told me that they are happy with your recovery considering how sick you were a few days ago. There is infection in your liver, they are doing further tests to rule out any serious problem and if everything is good, you’ll be moving out of ICU into the ward. He said that ICU patients normally have sleeping problems and were confused when they wake up. The recovery will be a long time.
Friday, 5th of September 2015 – Day 18
We went to see you around 9am, and arrived at 10:20. I brought you two towels, tooth brush and tooth paste, moisturiser and deodorant.
When I got in, you look better than yesterday. But still your eyes look so big and you look so thin, you just look different. There was no smile in your face. You asked me to put my hand on your eyes and again you let out happy sigh “nice”.
The doctor came to you and said that your liver number looks fine, they will be ready to move you to the normal ward so you can have better rest. The doctor asked “do you know the time?” You said “no”, the doctor said it’s “10:30 in the morning” you said “wow”.
I got a voice message from your nurse saying that you were moved to 5th floor, East wing ward this afternoon.
Saturday, 6th of September 2015 – Day 19
We went to Alfred hospital this morning, arriving about 10:30. You have got your own ward room facing north and you look better today. You told me you had a broken sleep last night (it’s better than not getting sleep in ICU). You told me that the doctor said you’ll stay in hospital (or bed) for 3 weeks time.
Sunday, 7th of September 2015 – Day 20
This was fathers day, and the first fully-cognitive day that I remember fully. My fiancé bought our daughter along to visit and we read through the get-well cards. At the time I had no recollection, other than memories of delirium, of my time in ICU. I seemed disconnected from the events that had taken place. I had no memory of pain or discomfort from the tubes, injections and the ECMO machine – just the scars to prove it.
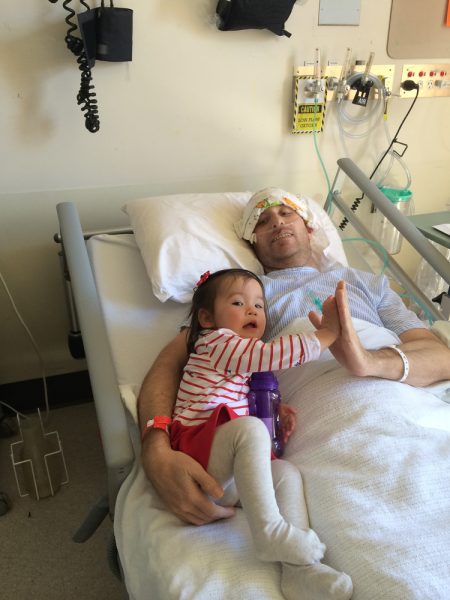
I had gone from a pre-illness weight of about 94kg to just under 80kg. My muscles had atrophied and I was unable to walk. It would take me a full week of rehab to start with standing, then shuffling a few steps with a frame, to managing to walk 20-50m with a walking frame. My right foot had temporary nerve damage from being on my back for so long and compressed nerves in my lower spine.
I spent the next 2 weeks in the ward, initially recovering from the intense delirium that the ICU drugs caused. The way I’ve explained this to others is that it was “like someone put your brain in a microwave for two minutes”. Since I have no memory of pain or discomfort from the time I spent in ICU, my real “trauma” was psychological. I can’t overstate how powerful the delirium was. It will be some time before those “memories” fade.
There were 3 core themes to my delirium:
- Playstation.
I don’t know where this “Playstation” thread seeded itself in my mind. I remember thinking that it started as a way of waiting during my initial stay in Knox hospital where I found a Virtual Reality version of a Playstation console (completely non-existent of course), this evolved (like a dream) to where I was aware that I was in a hospital, and that the Playstation technology had evolved into a 3D recorder and projection system was installed into the ICU room’s ceiling (see photo above with the nurse holding my daughter – the machines above me became the hardware of this delirium) and that it could directly influence my thinking and reality.
It’s hard to explain all of the massively intricate detail and sub-threads of this particular theme – but was so disturbing and prolonged, affecting my sleep, that the anaesthesiologist proscribed me with specific drugs to “block out” any Playstation visualisations.
- False Reality with Actors.
This was a particularly powerful “reality” where I was either observant or participating in other people (or myself) being drug-induced into acting out hero/villain roles that were supported by a cast of actors that were in on the reality and tried to aid in the downfall, or extraction of information. It had a ‘ground-hog day’ quality to it where scenes were recreated to optimise the outcome if it was unsuccessful.
Again a hard to explain, with this psuedo-dream lasting for many days.
- Death in the Family.
Probably the most emotional theme, and one that crossed-over a from conscious to sub/un-consciousness and reality. Knowing that I was in ICU I had the thought that my fiance’s family was travelling from overseas to visit me. As the time drew near for them to enter the room I was in, I heard a scream and for some reason the visit was postponed. I learned and deduced that a member of the family had become seriously ill. This delirium-based reality then saw that it was my fiance’s mother that had died of a heart attack from the stress and anxiety of the visit. This ‘reality’ progressed further to where I remember a memorial scene (in the hospital no less).
Most disturbing was that when my fiance’s sister arrived to visit (in reality, not as part of the delirium) and I was beginning to wake a little, I was still unable to distinguish from the delirium thoughts and reality, and was tearful and commiserating – to a somewhat bewildered set of family visitors.
It’s almost impossible to go into all of the detail of these delirium-based memories – they were real to me at the time and very hard to rationalise as I lay in the hospital bed afterwards. There were other little more minor thoughts and memories as well. So while I’ve said I lost those 19 days, it’s probably more accurate to say that I was swept away by thoughts and memories that never existed except as dreams so powerful that their imprint was seared into my mind.
While I was the one that endured the physical aspects of this life experience, it was my loved ones that suffered the emotional toll. My body is healing quickly – those emotional scars will take much longer.
EXIF:
